Endometriosis
- What is endometriosis?
- What are the symptoms of endometriosis?
- Who usually gets endometriosis?
- What can raise my chances of getting endometriosis?
- How can I reduce my chances of getting endometriosis?
- Why do patches of endometriosis cause pain and health problems?
- Why is it important to find out if I have endometriosis?
- How would I know if I have endometriosis?
- What causes endometriosis?
- How is endometriosis treated?
- How do I cope with a disease that has no cure?
See also:
What is endometriosis?
Endometriosis is a common health problem in women. It gets its name from the word endometrium, the tissue that lines the uterus (womb). In women with this problem, tissue that looks and acts like the lining of the uterus grows outside of the uterus in other areas. These areas can be called growths, tumors, implants, lesions, or nodules.
Most endometriosis is found:
- on or under the ovaries
- behind the uterus
- on the tissues that hold the uterus in place
- on the bowels or bladder
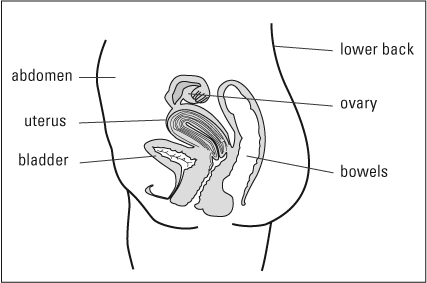
Endometriosis rarely grows in the lungs or other parts of the body. This "misplaced" tissue can cause pain, infertility (not being able to get pregnant), and very heavy periods.
What are the symptoms of endometriosis?
Pain is one of the most common symptoms of endometriosis. Usually the pain is in the abdomen, lower back, and pelvis. The amount of pain a woman feels does not depend on how much endometriosis she has. Some women have no pain, even though their disease affects large areas. Other women with endometriosis have severe pain even though they have only a few small growths. Symptoms of endometriosis include:
- Very painful menstrual cramps
- Pain with periods that gets worse over time
- Chronic pain in the lower back and pelvis
- Pain during or after sex
- Intestinal pain
- Painful bowel movements or painful urination during menstrual periods
- Heavy and/or long menstrual periods
- Spotting or bleeding between periods
- Infertility (not being able to get pregnant)
- Fatigue
Women with endometriosis may also have gastrointestinal problems such as diarrhea, constipation, or bloating, especially during their periods.
Who usually gets endometriosis?
About five million women in the United States have endometriosis. This makes it one of the most common health problems for women.
In general, women with endometriosis:
- get their monthly period
- are 27-years-old on average
- have symptoms for two to five years before finding out they have the disease
Women who have gone through menopause (when a woman stops having her period) rarely still have symptoms.
What can raise my chances of getting endometriosis?
You are more likely to develop endometriosis if you:
- began getting your period at an early age
- have heavy periods
- have periods that last more than seven days
- have a short monthly cycle (27 days or less)
- have a close relative (mother, aunt, sister) with endometriosis
How can I reduce my chances of getting endometriosis?
Some studies suggest that you may lower your chances of developing endometriosis if you:
- exercise regularly
- avoid alcohol and caffeine
Why do patches of endometriosis cause pain and health problems?
Growths of endometriosis are almost always benign or not cancerous, but still can cause many problems. To see why, it helps to understand a woman's monthly cycle. Every month, hormones cause the lining of a woman's uterus to build up with tissue and blood vessels. If a woman does not get pregnant, the uterus sheds this tissue and blood. It comes out of the body through the vagina as her menstrual period.
Patches of endometriosis also respond to a woman's monthly cycle. Each month the growths add extra tissue and blood, but there is no place for the built-up tissue and blood to exit the body. For this reason, growths tend to get bigger and the symptoms of endometriosis often get worse over time.
Tissue and blood that is shed into the body can cause inflammation, scar tissue, and pain. As the misplaced tissue grows, it can cover or grow into the ovaries and block the fallopian tubes. This can make it hard for women with endometriosis to get pregnant. The growths can also cause problems in the intestines and bladder.
Why is it important to find out if I have endometriosis?
The pain of endometriosis can interfere with your life. Studies show that women with endometriosis often skip school, work, and social events. This health problem can also get in the way of relationships with your partner, friends, children, and co-workers. Plus, endometriosis can make it hard for you to get pregnant.
Finding out that you have endometriosis is the first step in taking back your life. Many treatments can control the symptoms. Medicine can relieve your pain. And when endometriosis causes fertility problems, surgery can boost your chances of getting pregnant.
How would I know if I have endometriosis?
If you think you have this disease, talk with your obstetrician/gynecologist (OB/GYN). Your OB/GYN has special training to diagnose and treat this condition. The doctor will talk to you about your symptoms and health history. Then she or he will do a pelvic exam. Sometimes during the exam, the doctor can find signs of endometriosis.
Usually doctors need to run tests to find out if a woman has endometriosis. Sometimes doctors use imaging tests to "see" large growths of endometriosis inside the body. The two most common imaging tests are:
- ultrasound, which uses sound waves to see inside the body
- magnetic resonance imaging (MRI), which uses magnets and radio waves to make a "picture" of the inside of the body
The only way to know for sure if you have endometriosis is to have a surgery called laparoscopy. In this procedure, a tiny cut is made in your abdomen. A thin tube with a light is placed inside to see growths from endometriosis. Sometimes doctors can diagnose endometriosis just by seeing the growths. Other times, they need to take a small sample of tissue, or a biopsy, and study it under a microscope.
What causes endometriosis?
No one knows for sure what causes this disease, but scientists have a number of theories.
They know that endometriosis runs in families. If your mother or sister has endometriosis, you are six times more likely to get the disease than other women. So, one theory suggests that endometriosis is caused by genes.
Another theory is that during a woman's monthly periods, some endometrial tissue backs up into the abdomen through the fallopian tubes. This transplanted tissue then grows outside the uterus. Many researchers think a faulty immune system plays a part in endometriosis. In women with the disease, the immune system fails to find and destroy endometrial tissue growing outside of the uterus. Plus, a recent study shows that immune system disorders (health problems in which the body attacks itself) are more common in women with endometriosis. More research in this area may help doctors better understand and treat endometriosis.
How is endometriosis treated?
There is no cure for endometriosis, but there are many treatments for the pain and infertility that it causes. Talk with your doctor about what option is best for you. The treatment you choose will depend on your symptoms, age, and plans for getting pregnant.
Pain Medication. For some women with mild symptoms, doctors may suggest taking over-the-counter medicines for pain. These include: ibuprofen (Advil and Motrin) or naproxen (Aleve). When these medicines don't help, doctors may advise using stronger pain relievers available by prescription.
Hormone Treatment.When pain medicine is not enough, doctors often recommend hormone medicines to treat endometriosis. Only women who do not wish to become pregnant can use these drugs. Hormone treatment is best for women with small growths who don't have bad pain.
Hormones come in many forms including pills, shots, and nasal sprays. Many hormones are used for endometriosis including:
- Birth control pills block the effects of natural hormones on endometrial growths. So, they prevent the monthly build-up and breakdown of growths. This can make endometriosis less painful. Birth control pills also can make a woman's periods lighter and less uncomfortable. Most birth control pills contain two hormones, estrogen and progestin. This type of birth control pill is called a "combination pill." Once a woman stops taking them, the ability to get pregnant returns, but so may the symptoms of endometriosis.
- Progestins or progesterone medicines work much like birth control pills and can be taken by women who can't take estrogen. When a woman stops taking progestins, she can get pregnant again. But, the symptoms of endometriosis return too.
- Gonadotropin releasing hormone agonists or GnRH agonists slow the growth of endometriosis and relieve symptoms. They work by greatly reducing the amount of estrogen in a woman's body, which stops the monthly cycle. Leuprolide (Lupron®) is a GnRH agonist often used to treat endometriosis. GnRH agonists should not be used alone for more than six months. This is because they can lead to osteoporosis. But if a woman takes estrogen along with GnRH agonists, she can use them for a longer time. When a woman stops taking this medicine, monthly periods and the ability to get pregnant return. But, usually the problems of endometriosis also return.
- Danazol is a weak male hormone. Nowadays, doctors rarely recommend this hormone for endometriosis. Danazol lowers the levels of estrogen and progesterone in a woman's body. This stops a woman's period or makes it come less often. Danazol also gives pain relief. But it often causes side effects like oily skin, weight gain, tiredness, smaller breasts, and hot flashes. Danazol does not prevent pregnancy and can harm a baby growing in the uterus. Since it can't be used with other hormones, like birth control pills, doctors recommend using condoms, diaphragms, or other "barrier" methods to prevent pregnancy.
Surgery. Surgery is usually the best choice for women with endometriosis who have a severe amount of growths, a great deal of pain, or fertility problems. There are both minor and more complex surgeries that can help. Your doctor might suggest one of the following:
- Laparoscopy can be used to diagnose and treat endometriosis. During this surgery, doctors remove growths and scar tissue or destroy them with intense heat. The goal is to treat the endometriosis without harming the healthy tissue around it. Women recover from laparoscopy much faster than from major abdominal surgery.
- Laparotomy or major abdominal surgery is a last resort treatment for severe endometriosis. In this surgery, the doctor makes a much bigger cut in the abdomen than with laparoscopy. This allows the doctor to reach and remove growths of endometriosis in the pelvis or abdomen. Recovery from this surgery can take up to two months.
- Hysterectomy should only be considered by women who do not want to become pregnant in the future. During this surgery, the doctor removes the uterus. She or he may also take out the ovaries and fallopian tubes at the same time. This is done when the endometriosis has severely damaged them.
How do I cope with a disease that has no cure?
You may feel many emotions—sadness, fright, anger, confusion, and loneliness. It is important to get support to cope with endometriosis. Consider joining a support group to talk with other women who have endometriosis. There are support groups on the Internet and in many communities.
It is also important to learn as much as you can about the disease. Talking with friends, family, and your doctor can help.
For More Information...
You can find out more about endometriosis by contacting the National Women's Health Information Center (NWHIC) at 1-800-994-9662 or the following organizations:
Endometriosis Association
Phone Number(s): (414) 355-2200
Internet Address: http://www.endometriosisassn.org/
The American College of Obstetricians and Gynecologists
Phone Number(s): (800) 762-2264 x 192 (for publication requests only)
Internet Address: http://www.acog.org/
Endometriosis Research Center
Phone Number(s): (800) 239-7280
Internet Address: http://www.endocenter.org/

